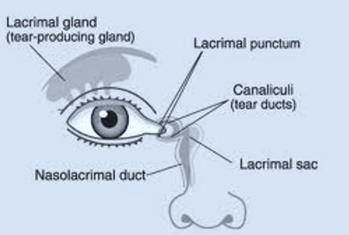
The majority of tears are produced in the lacrimal gland, which is located in a recessed area within the upper outside portion of the orbit.
Tears drain by traveling across the eye toward the nose into tiny holes in the upper and lower eyelid margins called punctae, travel through upper and lower canaliculi (tubes) in the lids, collect in a common canaliculus, move into the lacrimal sac and enter the nose through the nasolacrimal duct.
What are the Symptoms of Nasolacrimal Duct Obstruction?
If this pathway is obstructed or blocked, excess tearing (epiphora), discharge, crusting, and red lids (from being wet and repeatedly rubbed or wiped) can result.
What are the Causes of Nasolacrimal Duct Obstruction?
Congenital blockages along this pathway most commonly occur because a membrane (the valve of Hasner) across the bottom of the duct fails to open at or around the time of birth and obstructs drainage.
Alternatively, tear flow may be blocked at any other point along the passageway, for example, because of absent or stenotic puncta(e); abnormal inferior or superior canaliculi; abnormal communication between the canaliculi of the lids to the common canaliculus or between the common canaliculus and the lacrimal sac; or because of a narrow, crooked, or bony duct termination.
Nasolacrimal Duct Obstruction Diagnosis
A dye disappearance test can confirm the diagnosis. A drop of fluorescein is placed on the symptomatic eye(s). The drop should drain completely in five minutes. If not, the test is positive.
Epiblepharon of the lower lid, a condition in which a horizontal fold of eyelid muscle and skin push eyelashes of the lower lid upward to the point they are vertical and sometimes rub the eye, may confound the interpretation of this test and may cause excess tears to persist despite nasolacrimal duct probing.
How do you Treat Nasolacrimal Duct Obstruction?
Conservative
- Nasolacrimal duct massage
Place a fingertip over the common canaliculus/lacrimal sac and apply pressure in an inward and then downward direction along the side of the nose. Dr. Shin uses the analogy of milking the contents of a frosting bag through a clogged tip. - Aquaphor may be applied to the skin overlying the area to be massaged (to avoid causing the child’s fragile skin to become red).
- Ophthalmic antibiotic eye drops may be instilled, if yellowish/greenish discharge and crusting are present, prior to massage multiple times in a row. If the discharge resolves, but the child still has excessive tearing, the parents/caretakers are to discontinue the drops but to continue massage of the affected area.
- Ophthalmic antibiotic ointment may be prescribed for red, chapped lids.
Surgery
- Nasolacrimal duct probing with irrigation of the lacrimal drainage system.
Most often the condition resolves in the first year of life; however, if symptoms do not respond to conservative management, nasolacrimal duct probing is usually indicated.
This procedure is performed in an ambulatory surgery center. The child is placed under general anesthesia and monitored by an anesthesiologist. The procedure takes 5 minutes for one eye and 10 minutes for both eyes.
It may take a few days for the child’s symptoms to improve. Eye and nose drops will be used for two weeks after surgery.








